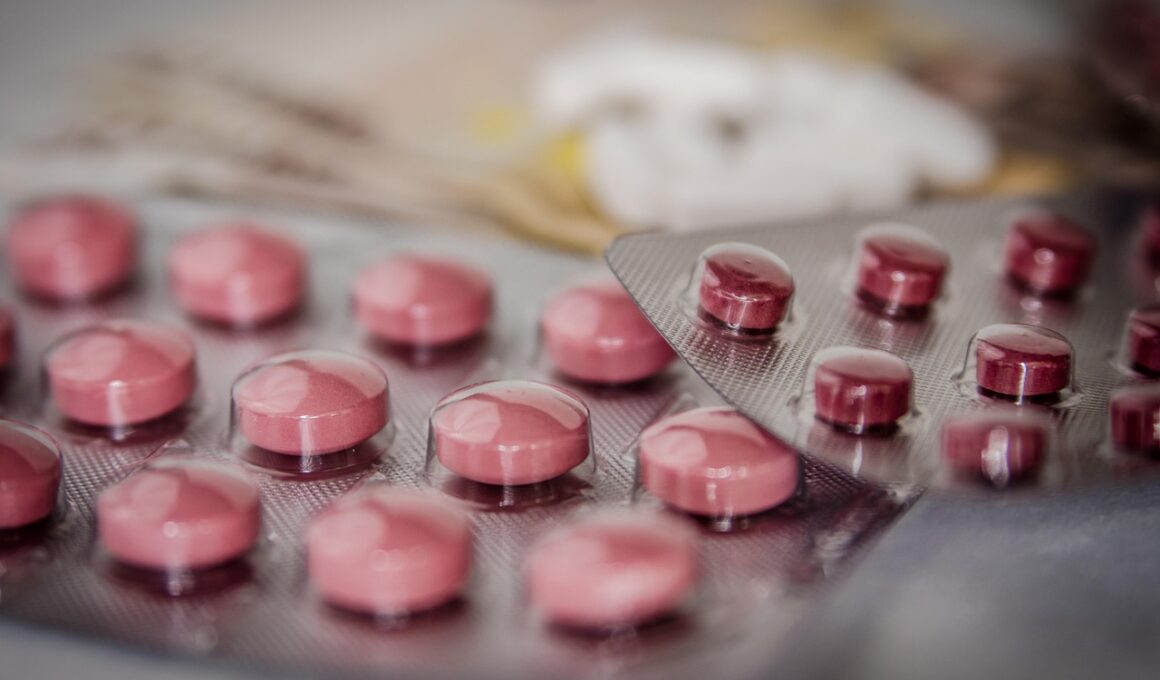
Psychiatric Medication Interactions: What to Watch For
Psychiatric medications play a critical role in managing mental health issues. However, they can sometimes have complex interactions with other medications, foods, and lifestyle choices. Understanding these interactions is essential for patients and healthcare providers alike. It is vital to communicate openly about all medications being taken, including over-the-counter and herbal supplements. Patients often forget to mention these, but they can dramatically affect treatment outcomes. Some interactions may be mild, while others can lead to severe side effects or reduced efficacy of drugs. For example, combining certain antidepressants with specific pain relievers can increase the risk of serotonin syndrome. Other substances, like alcohol, can also interfere with how psychiatric medications work. Individuals should also be conscious of how over-the-counter medications impact their current prescriptions. Keeping a comprehensive list of all substances being consumed can aid doctors in providing the safest treatment options. Regular check-ins with healthcare professionals are advised to review all medications and make necessary adjustments.
One common class of psychiatric medications, antidepressants, often interacts with various other medications. Selective serotonin reuptake inhibitors (SSRIs), often prescribed for depression, can have significant interactions with certain pain medications and anticoagulants. For instance, when SSRIs are taken with NSAIDs, they can increase the risk of gastrointestinal bleeding. This warning is critical for anyone needing pain management while being treated for depression or anxiety. Additionally, the metabolism of certain medications, such as antipsychotics, can be affected by other drugs that inhibit or induce liver enzymes. Patients on antipsychotics should be particularly cautious when taking medications like certain antibiotics or antifungals, which can alter their medication levels. It is always advisable to consult a healthcare provider about using multiple medications simultaneously and to understand potential risks. As many individuals may also use herbal supplements or alternative treatments, it is crucial to inform healthcare professionals about these as well. Doing so can help avoid adverse effects and ensure the prescribed treatment is effective.
Understanding Food Interactions
Food can also impact the effectiveness of psychiatric medications significantly. Certain foods might boost or inhibit how these medications work. Grapefruit juice, for example, is notorious for its ability to alter the metabolism of various medications, including some psychiatric ones. When someone takes medications that interact with grapefruit juice, it could lead to higher concentrations of the drug in the bloodstream, increasing side effects. This can be particularly concerning for individuals taking medications for anxiety or depression. Similarly, tyramine-rich foods, like aged cheeses or cured meats, can interact with monoamine oxidase inhibitors (MAOIs), leading to dangerous spikes in blood pressure. Patients on these medications must adhere to strict dietary restrictions to avoid serious reactions. Maintaining an open dialogue with healthcare providers about diet is essential for anyone taking psychiatric medications. This includes discussing preferred food choices, any recent dietary changes, and how these might affect their medication regimen. Being proactive in these discussions can prevent potential complications down the line.
Herbal supplements can also pose serious risks when taken alongside psychiatric medications. Common herbs like St. John’s Wort, for instance, are often touted for their mood-enhancing properties but can interfere with prescribed antidepressants. When combined, St. John’s Wort can reduce the effectiveness of these medications, potentially worsening the patient’s condition. Given the increased interest in natural remedies, patients should be educated about the potential risks of mixing herbal supplements with psychiatric medications. Clear guidelines should be established for healthcare providers to discuss alternative medicine products and their interactions with prescribed treatments. Many patients may feel that herbal supplements are safer options since they are ‘natural,’ but this is not always the case. Professional guidance is essential in navigating any supplement’s impact on mental health treatment. Moreover, clinicians should remain updated on common herbal supplements their patients might be consuming. Setting up a thorough screening system can ensure that all substance uses are identified and accounted for in creating a safe treatment plan for mental health issues.
The Importance of Monitoring Medication Effects
Continuous monitoring of medication interactions is crucial for effective psychiatric treatment. Regular follow-ups give healthcare providers the opportunity to evaluate how well the medications work and if any side effects are present. During these visits, both the patient and the provider can discuss any newfound medications, adjustments, or lifestyle changes affecting drug efficacy. Medication blood levels need to be monitored, especially for drugs with a narrow therapeutic range. Patients must feel comfortable raising any concerns about their treatment outcomes, like changes in mood, energy levels, or physical health. Research suggests that actively involving patients in their medication management can lead to better treatment adherence and outcomes. Educational programs about medication interactions and their implications for mental health should be readily available. These programs can empower patients to participate actively in their treatment decisions. Cultivating awareness, trust, and communication between patients and providers enhances therapeutic relationships and encourages the patient to take an active role in managing their mental health.
Patients should also be aware of how lifestyle factors influence psychiatric medication interactions. Elements like sleep patterns, exercise, and stress levels can all play roles in how well medications work. For example, sleep deprivation can exacerbate mental health conditions or decrease medication efficacy. Similarly, not maintaining a balanced diet may affect patients’ overall well-being. Encouraging regular physical activity has been shown to improve mental health outcomes and might also mitigate some medication-related issues. Patients should be educated about the significance of maintaining a healthy lifestyle while undergoing treatment. Additionally, establishing daily routines can help mitigate stress and maximize medication benefits. Interventions promoting lifestyle modifications can empower individuals by placing them in control of their mental health. Mental health professionals should consider incorporating holistic approaches combining lifestyle coaching and medication management for comprehensive care. This integrated approach acknowledges that mental health is multifactorial and often requires looking beyond medications alone to achieve optimal outcomes.
Conclusion on Psychiatric Medications
Understanding psychiatric medication interactions is essential for ensuring the best possible treatment outcomes. Patients must feel empowered to communicate openly with their healthcare providers regarding dietary habits, other medications, and lifestyle choices. Clinicians should remain vigilant in monitoring these interactions. Regular follow-ups, thorough assessments, and patient education can prevent negative outcomes associated with medication interactions. Awareness of potential risks from herbal supplements and foods can further enhance treatment adherence and efficacy. It is also crucial to recognize that psychiatric medications are only part of a holistic treatment plan that includes lifestyle modifications and emotional support. Ongoing research aims to uncover more about these interactions, helping create better safety guidelines for using these essential drugs. As mental health treatment continues evolving, an increasing emphasis on patient education will likely significantly improve therapeutic effectiveness. A collaborative approach combining the expertise of both the patient and healthcare provider creates opportunities for success in managing mental health conditions. By understanding interactions and proactively addressing them, individuals can achieve better mental health outcomes.
Resources for Further Learning
For those interested in deeper learning about psychiatric medications, their interactions, and mental health management, various resources are available online. Websites from established health organizations, such as the National Institutes of Health or the American Psychiatric Association, provide reliable and extensive information on medications and their impacts. Many of these organizations also offer educational materials tailored to patients, helping demystify complex medical information. Local support groups can also serve as valuable resources; connecting with others facing similar challenges fosters a sense of community. Such groups often share personal insights into managing medication interactions and side effects and provide emotional support. Additionally, mental health apps can offer medication management tools, reminders, and educational resources directly accessible on smartphones. These applications ensure patients are compliant with their treatment plans while receiving information on side effects and drug interactions. Pharmacists, too, play a vital role in this educational process by advising on prescription medications and helping navigate potential interactions. Establishing a supportive network of healthcare professionals, community resources, and technology can significantly enhance one’s understanding of medication interactions.