Common Gut Microbiome Disorders and Their Nutritional Management
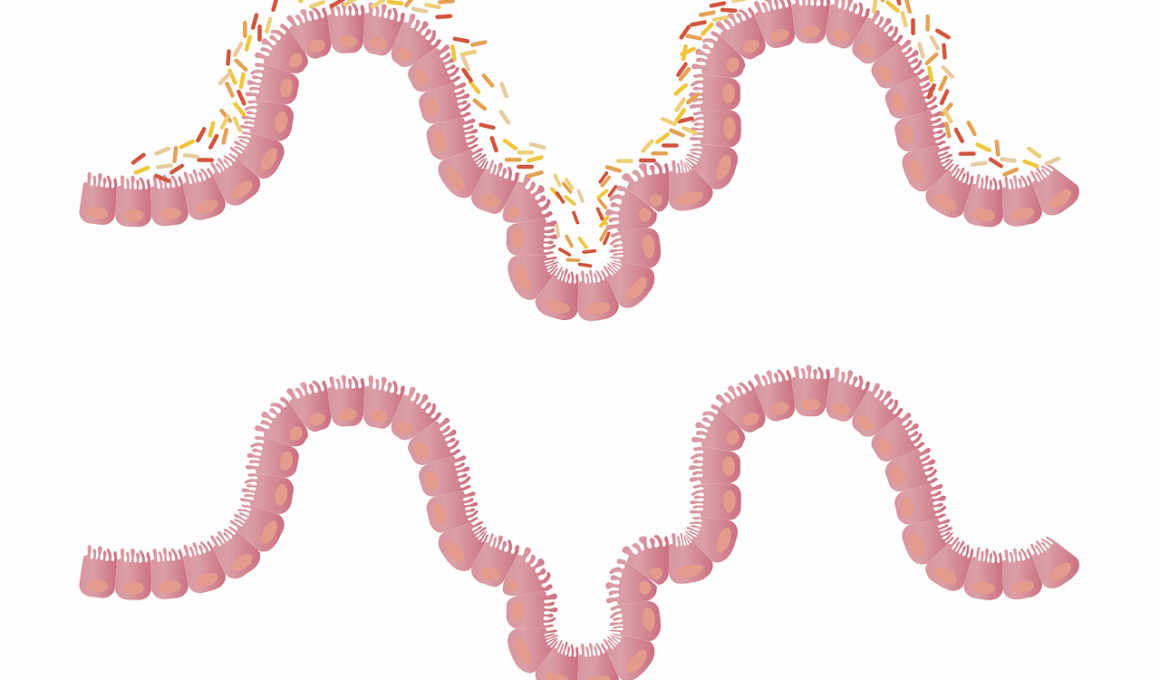
The gut microbiome plays a critical role in overall health and well-being. A diverse and balanced gut microbiome contributes to digestion, nutrient absorption, and immune function. However, various gut microbiome disorders can develop, leading to digestive issues and other health problems. These disorders are often associated with poor dietary choices, stress, and antibiotic use. Understanding these disorders, such as dysbiosis, irritable bowel syndrome (IBS), and inflammatory bowel disease (IBD), is essential for effective nutritional management. Dysbiosis is a microbial imbalance that can lead to various gastrointestinal symptoms. IBS affects a large population and causes abdominal pain and altered bowel habits. IBD is a more severe condition, comprising Crohn’s disease and ulcerative colitis, necessitating comprehensive management. Nutrition plays a pivotal role in treating these disorders. Addressing gut dysbiosis involves dietary modulation, including increasing fiber intake, reducing processed foods, and incorporating fermented foods. These changes can promote a healthier microbiome composition, reducing symptoms. Therefore, recognizing the importance of nutrition in gut health is crucial for optimal management and supporting the microbiome’s health.
Dysbiosis: Causes and Nutritional Strategies
Dysbiosis refers to an imbalance of gut bacteria, often contributing to several gastrointestinal disorders. Factors leading to dysbiosis include an unhealthy diet, stress, excessive alcohol intake, and antibiotic use. These disrupt the natural microbiota balance, paving the way for harmful bacteria to proliferate. Symptoms of dysbiosis can range from bloating and abdominal pain to food intolerances. Nutritional management begins with identifying food patterns that may worsen symptoms. Emphasizing whole foods rich in fiber, such as fruits and vegetables, is crucial. Incorporating probiotics and prebiotics can also support rehabilitation by promoting healthy bacterial growth. Additionally, fermented foods like yogurt, kefir, and sauerkraut introduce beneficial microbes to the gut. Reducing sugar and refined carbohydrate intake can help minimize dysbiosis symptoms further. This dietary shift helps reinforce the gut barrier, enhancing immunity and overall gut health. It’s essential to personalize the diet based on individual responses, as not all foods suit everyone. Consulting with a healthcare professional or registered dietitian can aid in creating an effective nutrition plan tailored to specific needs.
Irritable bowel syndrome (IBS) is characterized by recurrent abdominal pain, discomfort, and altered bowel habits, affecting millions worldwide. Although its precise causes remain unknown, a combination of factors, including altered gut motility, visceral hypersensitivity, and psychosocial aspects, play a role. Additionally, dietary intake significantly influences IBS symptoms, making nutritional management vital. Certain foods may trigger symptoms, prompting individuals to identify and eliminate triggers. Common dietary triggers include high-fat foods, dairy, alcohol, and some carbohydrates known as FODMAPs. A low-FODMAP diet has gained popularity in managing IBS, as it helps reduce symptoms for many affected individuals. This approach involves temporarily eliminating high-FODMAP foods and gradually reintroducing them to identify personal triggers. To support digestion, incorporating soluble fiber sources is beneficial. Foods like oats, bananas, and carrots can help regularize bowel movements. Staying hydrated and managing stress through relaxation techniques also positively impact IBS management. Individual variation is paramount, emphasizing the need for a personalized dietary strategy. Collaborating with healthcare providers can facilitate optimal symptom control through a well-structured nutrition plan.
Inflammatory Bowel Disease: Dietary Considerations
Inflammatory bowel disease (IBD) encompasses chronic conditions including Crohn’s disease and ulcerative colitis, leading to significant inflammation of the gastrointestinal tract. Globally, these conditions affect millions, and nutritional management plays a crucial role. Key symptoms include abdominal pain, diarrhea, weight loss, and fatigue, which can significantly impact quality of life. Nutritional therapy aims to address these symptoms and support the patient’s nutritional status and overall health. During flare-ups, a low-residue diet may be recommended as it minimizes fiber intake to reduce digestive workload. This diet includes refined grains, dairy, and well-cooked vegetables while avoiding nuts and seeds. Identifying food sensitivities is essential for effective management, as certain foods can exacerbate symptoms. Implementing an anti-inflammatory diet promoting omega-3 fatty acids from sources like fish helps manage inflammation. Additionally, ensuring adequate protein intake is crucial for maintaining muscle mass, particularly in those experiencing weight loss. Regular monitoring of nutritional status is vital, as deficiencies can occur in IBD patients. Collaborating with a dietitian specializing in IBD can ensure a personalized, balanced dietary approach essential for managing chronic inflammation effectively.
The relationship between diet, gut health, and the microbiome is complex, and individualized approaches are vital for effective management of gut microbiome disorders. Engaging with a qualified healthcare provider in a comprehensive assessment will determine the best nutritional approach. Integrating a holistic view of health may also include addressing lifestyle factors such as sleep, physical activity, and stress management. Fiber is a significant dietary component promoting gut health; hence, increasing its intake from whole grains, legumes, fruits, and vegetables is crucial. Moreover, ensuring diversity in the diet can nurture a diverse microbiome, ultimately playing a beneficial role in health. Recommendations for regular consumption of prebiotics, found in onions, garlic, bananas, and oats, may aid in promoting beneficial bacteria. It is also crucial to limit processed foods and added sugars to support gut microbial health. Furthermore, staying adequately hydrated enhances digestive health, and herbal teas and probiotics may be beneficial adjuncts. Each individual’s response to dietary changes will vary, reinforcing the importance of continuous monitoring and adaptation of dietary strategies. Ultimately, fostering a supportive environment for a healthy gut microbiome will lead to improved health outcomes.
Conclusion: Emphasizing Nutritional Interventions
In conclusion, addressing common gut microbiome disorders through nutrition is paramount for optimal health. This approach emphasizes the interconnection between gut health, diet, and overall well-being. The disorders discussed, including dysbiosis, IBS, and IBD, reveal the importance of individualized dietary strategies in managing symptoms and enhancing quality of life. By focusing on whole, nutrient-dense foods, individuals may experience notable improvements in gut health and overall quality of life. Furthermore, as dietary interventions offer a practical and accessible avenue for management, patients are encouraged to engage in shared decision-making with healthcare providers. Implementing diverse dietary habits, including the incorporation of prebiotics and probiotics, is essential in nurturing a thriving gut microbiome. Additionally, regular follow-ups can help tailor dietary approaches to individual needs, adapting changes as necessary. Ultimately, cultivating awareness of food choices and their impact on gut health empowers individuals in their journey toward improved health. Integrating dietary changes with appropriate support can lead to a successful outcome, fostering a balanced microbiome and enhancing well-being significantly.
In summary, recognizing the influence of nutrition on gut microbiome health is crucial for managing disorders effectively. The interplay between diet, lifestyle factors, and gut health cannot be overlooked. It is equally important to stay updated with emerging research in this field, as our understanding of the gut microbiome continues to evolve. Practical takeaways include focusing on whole foods, increasing fiber intake, and being mindful of potential trigger foods. Individual variability warrants the need for personalized dietary strategies, encouraging individuals to keep food diaries or seek professional guidance when needed. Education around the importance of gut health can inspire proactive engagement in optimizing diet and lifestyle. Continued advancements in scientific literature aim to shed light on the microbiome’s influence on various health conditions, fostering a culture of better health through informed decisions. Ultimately, enhancing gut microbiome health can positively impact physical and mental well-being, demonstrating the profound connection between body and mind. A commitment to nutritious eating habits encourages lasting changes, promoting a flourishing microbiome and paving the way for improved health outcomes.
Practical Tips for Improving Gut Microbiome Health
A practical approach to promoting gut microbiome health involves several actionable tips. First, involving gradual changes in dietary habits helps individuals adapt better. This may include introducing more whole foods and reducing reliance on processed options. Second, diversifying dietary choices ensures the inclusion of various nutrients. Each type of bacteria thrives on different foods, so incorporating a wide range of foods can promote microbial diversity. Third, staying hydrated supports digestion and overall health. Drinking sufficient water throughout the day enhances nutrient absorption and helps prevent constipation. Fourth, regular physical activity has been shown to benefit gut health. Exercise can positively influence the composition of gut microbiota and improve digestive function. Fifth, mindfulness practices, such as yoga or meditation, can help reduce stress, indirectly benefiting gut health. Logical sequencing of dietary changes, including keeping food diaries to track symptoms, can further assist individuals in identifying foods that work best for their gut. Lastly, including fermented foods in the diet can boost beneficial bacteria, creating a favorable balance in the microbiome. Following these tips cultivates a supportive environment for a healthier gut microbiome.